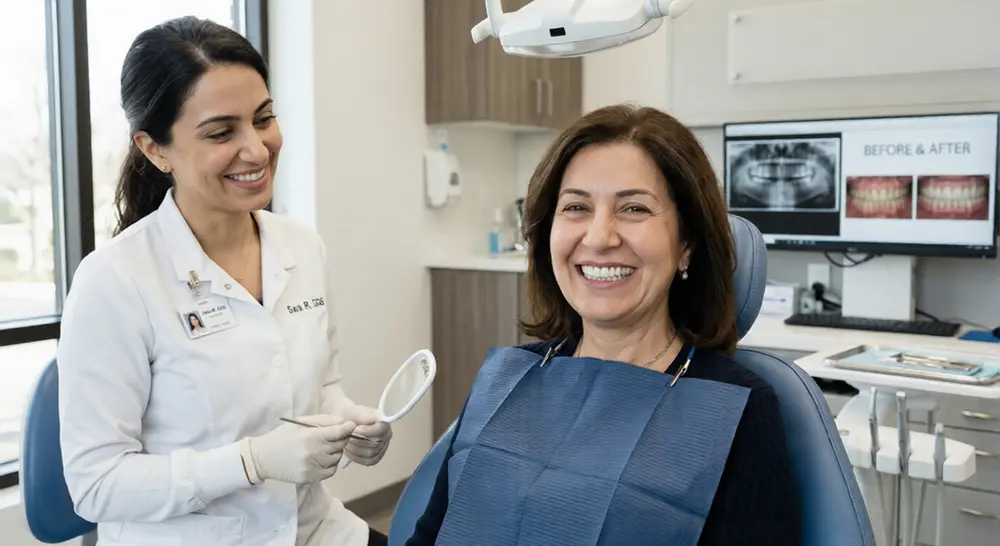
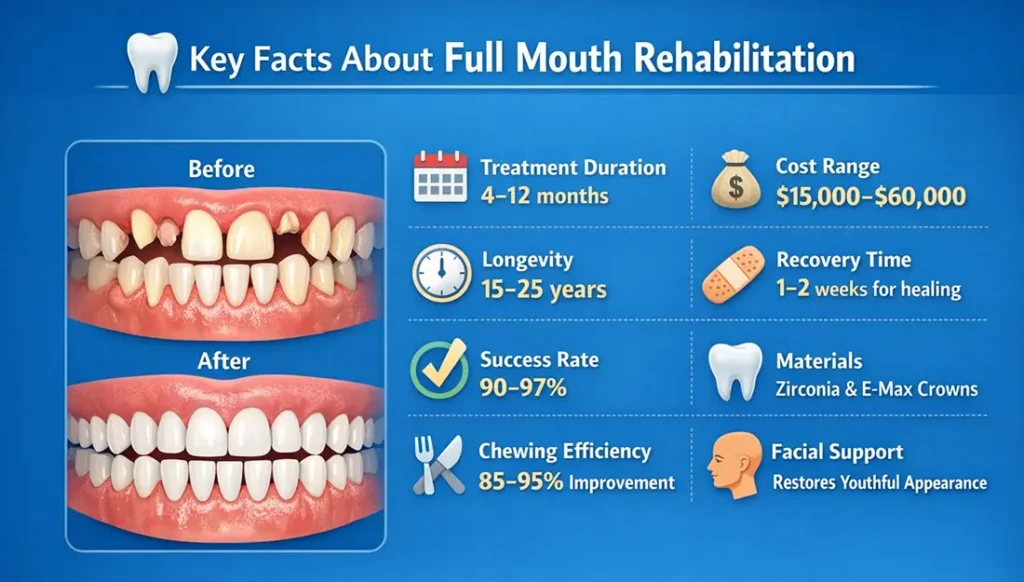
Full mouth rehabilitation restores worn, damaged, or missing teeth while rebuilding facial structure, jaw alignment, and oral function, often reversing visible signs of aging caused by bite collapse and tooth wear.
Many people notice facial aging long before they realize the real cause is dental structural loss. When teeth wear down, fracture, or go missing, the lower third of the face loses vertical support. The chin moves closer to the nose. Lips collapse inward. Wrinkles deepen. Jaw joints strain. This is not cosmetic alone. It is structural deterioration.
“It’s not just a dental procedure; it’s a non-surgical facelift that restores the skeletal support your skin needs to look firm and youthful.”
Full mouth rehabilitation, also called full mouth reconstruction or oral rehabilitation, rebuilds the bite system. It restores teeth, jaw relationships, and facial support simultaneously.
Clinical research confirms that restoring vertical dimension improves facial balance, chewing efficiency, and patient-reported quality of life. A 2019 systematic review in the Journal of Oral Rehabilitation reported significant improvement in function, muscle comfort, and facial aesthetics following occlusal rehabilitation.
This treatment involves prosthodontics, implant dentistry, restorative dentistry, and digital diagnostics working together.
Patients with severe tooth wear, bone loss, or multiple missing teeth often benefit from full mouth rehabilitation to restore structural stability and facial support.
What is Full Mouth Rehabilitation (FMR)?
Full mouth rehabilitation is the complete restoration of all teeth and bite relationships using crowns, implants, bridges, or prosthetics to rebuild oral function, jaw alignment, and facial structure.
Full mouth rehabilitation differs from isolated treatments. Instead of repairing individual teeth, it restores the entire chewing system.
This includes:
- Occlusal rehabilitation
- Full mouth crowns
- Dental implants
- Full arch reconstruction
- Implant-supported dentures
- Bite correction
- Jaw stabilization
The treatment falls under dental prosthodontics, a specialty focused on restoring and replacing teeth.
Research published in Clinical Oral Implants Research (2021) found implant-supported full arch restorations demonstrated survival rates above 95% over 10 years.
Full mouth rehabilitation restores structural integrity while protecting remaining natural teeth.
Full Mouth Rehabilitation vs Full Mouth Reconstruction: What Is the Real Difference?
Full mouth rehabilitation vs full mouth reconstruction describe the same clinical process but emphasize slightly different goals.
Full mouth rehabilitation focuses on restoring function, muscle balance, and joint stability.
Full mouth reconstruction focuses on rebuilding damaged or missing dental structures.
Both involve:
- Implant dentistry
- Crown and bridge restoration
- Occlusal rehabilitation
- Prosthetic reconstruction
The goal is restoring structural and functional stability.
Cosmetic dentistry improves appearance only. Full mouth rehabilitation restores structural health.
Who Needs Full Mouth Rehabilitation and Why Does It Become Necessary?
Full mouth rehabilitation is necessary when widespread dental damage affects multiple teeth, bite alignment, or jaw function.
Common causes include:
- Severe bruxism (teeth grinding)
- Acid erosion from reflux or diet
- Tooth wear from aging
- Trauma
- Bone loss
- Congenital conditions
- Failed dental restorations
Full mouth rehabilitation for bruxism restores worn tooth structure while protecting against future grinding damage.
Patients with severe tooth wear often experience loss of vertical dimension. This shortens facial height and accelerates facial aging.
Patients missing multiple teeth may need implant-supported solutions such as implant-supported dentures for stability and function.
Full Mouth Rehabilitation for Bruxism (Teeth Grinding)
Full mouth rehabilitation for bruxism restores structural damage caused by chronic grinding while stabilizing bite forces and protecting remaining teeth.
Bruxism creates extreme mechanical stress. Bite forces during grinding can exceed 700 newtons, far higher than normal chewing forces.
This leads to:
- Flattened teeth
- Fractured crowns
- Jaw pain
- TMJ strain
- Muscle fatigue
Rehabilitation restores proper tooth anatomy and distributes forces evenly.
Night guards or full mouth splints protect restorations long-term.
Research published in Journal of Prosthetic Dentistry (2018) found occlusal rehabilitation significantly reduced muscle strain and restoration failure in bruxism patients.
Full Mouth Reconstruction for Acid Erosion Patients
Full mouth reconstruction for acid erosion patients restores teeth weakened by chemical erosion caused by gastric reflux, diet, or medical conditions.
Acid dissolves enamel, exposing dentin and weakening tooth structure.
This leads to:
- Sensitivity
- Tooth shortening
- Bite collapse
- Increased fracture risk
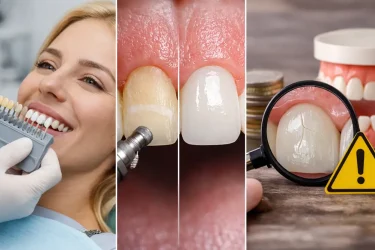
Restoration rebuilds lost enamel using crowns or veneers.
Severe cases require implant-supported reconstruction.
This restores bite stability and protects teeth from further erosion.
The Role of Occlusion and Bite Alignment in Oral Rehabilitation
Occlusion determines how forces distribute across teeth and jaw joints.
Misaligned bite relationships create uneven stress.
This causes:
- Tooth fractures
- TMJ dysfunction
- Muscle fatigue
- Bone loss
Occlusal rehabilitation restores balanced force distribution.
Neuromuscular dentistry evaluates muscle-guided jaw position.
Research in Journal of Oral Rehabilitation (2020) found correcting occlusion improved chewing efficiency and reduced TMJ symptoms.
Neuromuscular Dentistry in Full Mouth Rehabilitation
Neuromuscular dentistry in full mouth rehabilitation evaluates jaw position using muscle physiology instead of tooth contact alone.
This involves:
- Electromyography
- Jaw tracking
- Bite force measurement
This identifies optimal jaw alignment.
Restoring teeth in proper neuromuscular position improves comfort and reduces long-term strain.
Full Mouth Restoration for Patients with Bone Loss
Full mouth restoration for patients with bone loss rebuilds jaw structure using bone grafting and implant placement.
Bone loss occurs after tooth loss due to lack of stimulation.
Implants restore stimulation and prevent further bone deterioration.
Bone grafting restores implant support.
Patients with advanced bone loss may receive fixed hybrid dentures supported by implants.
Step-by-Step Full Mouth Reconstruction Process
Full mouth rehabilitation follows structured clinical phases.
Step-by-step full mouth reconstruction process includes diagnostic, surgical, restorative, and maintenance phases.
Phase 1: Diagnostic evaluation
Phase 2: Disease control
Phase 3: Implant placement or structural preparation
Phase 4: Temporary restorations
Phase 5: Final restorations
Each phase ensures structural stability and functional success.
Patients often begin with dental cleanings to stabilize gum health before reconstruction.
All-on-4 vs Traditional Full Mouth Rehabilitation: Which Is Better?
All-on-4 vs traditional full mouth rehabilitation is a critical decision because both treatments restore full dental function but differ in structure, healing time, and long-term biomechanics.
All-on-4 uses four dental implants to support a full arch prosthesis. Traditional full mouth rehabilitation may use individual implants, crowns, bridges, or combinations of treatments depending on the patient’s needs.
The differences are structural, functional, and biomechanical.
| Feature | All-on-4 Implants | Traditional Full Mouth Rehabilitation |
|---|---|---|
| Number of implants | 4 per arch | 6–10 per arch |
| Treatment time | Faster | Longer |
| Stability | High | Very high |
| Bone preservation | Good | Excellent |
| Customization | Moderate | Maximum |
| Longevity | 15–20 years | 20+ years |
All-on-4 works well for patients with significant tooth loss and moderate bone availability.
Traditional reconstruction provides the most customized and biomechanically optimized results, especially when preserving natural teeth or restoring complex bite relationships.
A long-term study published in Clinical Implant Dentistry and Related Research (2020) reported All-on-4 implant survival rates above 94% after 10 years.
Patients transitioning from removable prosthetics often benefit from dentures initially before converting to implant-supported full arch reconstruction.
Best Materials for Full-Mouth Dental Crowns and Bridges
Best materials for full mouth dental crowns must balance strength, aesthetics, wear resistance, and long-term structural stability.
The most common materials include:
Zirconia Restorations
Zirconia is currently the strongest and most fracture-resistant dental material.
Benefits include:
- Extremely high strength (900–1200 MPa flexural strength)
- Excellent wear resistance
- Long lifespan
- Biocompatibility
A 2021 study in Dental Materials found zirconia crowns demonstrated superior fracture resistance compared to porcelain-based restorations.
E-Max Lithium Disilicate
E-max provides exceptional aesthetics with high strength.
Best used in visible areas requiring natural appearance.
Porcelain Fused to Metal
Provides strength but less aesthetic quality compared to zirconia or E-max.
Material selection depends on:
- Bite force
- Location in mouth
- Bruxism risk
- Aesthetic goals
Full Mouth Rehabilitation for TMJ Disorders
Full mouth rehabilitation for TMJ disorders restores jaw alignment, improves bite stability, and reduces stress on jaw joints and muscles.
TMJ disorders often result from unstable bite relationships.
Symptoms include:
- Jaw pain
- Clicking
- Headaches
- Muscle fatigue
Occlusal rehabilitation corrects bite imbalance.
Neuromuscular alignment restores proper jaw positioning.
Research published in Journal of Prosthetic Dentistry (2019) showed bite correction reduced TMJ symptoms in over 70% of patients undergoing full rehabilitation.
Success Rate of Full Mouth Rehabilitation in Seniors
Success rate of full mouth rehabilitation in seniors remains extremely high when proper planning, implant integration, and maintenance protocols are followed.
Age alone does not prevent successful treatment.
Implant success rates remain above 90% even in patients over age 70.
Bone density and systemic health influence outcomes more than age itself.
A systematic review in International Journal of Implant Dentistry (2022) confirmed high survival rates of implant-supported full arch restorations in elderly patients.
Full mouth rehabilitation improves nutrition, speech, and overall quality of life.
Sedation Options for Full Mouth Dental Work
Sedation options for full mouth dental work allow complex treatment to be completed comfortably while minimizing patient stress and discomfort.
Available sedation methods include:
- Oral sedation
- Nitrous oxide sedation
- IV sedation
Sedation reduces anxiety, muscle tension, and procedural discomfort.
Patients remain relaxed throughout treatment.
Sedation dentistry improves treatment acceptance and patient experience.
Recovery Time After Full Mouth Restoration Surgery
Recovery time after full mouth restoration surgery varies depending on implants, bone grafting, and extent of reconstruction.
Typical recovery stages:
Initial healing: 1–2 weeks
Implant integration: 3–6 months
Final stabilization: 6–12 months
Most patients resume normal daily activities within a few days.
Temporary restorations maintain function during healing.
Complications of Full Mouth Reconstruction and How to Avoid Them
Complications of full mouth reconstruction are rare but can include implant failure, bite imbalance, or material fracture if proper planning and maintenance are not followed.
Potential complications include:
- Implant integration failure
- Bite misalignment
- Crown fracture
- Gum inflammation
Risk reduction strategies include:
- Digital bite analysis
- Proper implant placement
- Night guard protection
- Regular maintenance
Studies in Clinical Oral Implants Research (2021) report overall implant success rates exceeding 95%.
Full Mouth Reconstruction Before and After Expectations
Full mouth reconstruction before and after expectations should include improved function, structural stability, and natural appearance while understanding healing timelines and adaptation periods.
Expected improvements include:
- Improved chewing ability
- Restored facial support
- Reduced jaw pain
- Natural smile aesthetics
Temporary restorations allow patients to maintain appearance throughout treatment.
Digital planning improves predictability of results.
How to Finance Full Mouth Dental Restoration
How to finance full mouth dental restoration depends on treatment complexity, insurance coverage, and available payment options.
Common financing methods include:
- Dental insurance partial coverage
- Third-party dental financing
- Monthly payment plans
- Healthcare credit providers
Insurance may cover medically necessary components.
Cosmetic components typically require out-of-pocket payment.
Full Mouth Restoration for Patients with Bone Loss
Severe bone loss often occurs after tooth loss.
Bone grafting restores structural support.
Implants stimulate bone and prevent further deterioration.
Patients with severe bone loss benefit from implant-supported full arch restorations.
Long-Term Maintenance of Full Mouth Rehabilitation
Proper maintenance ensures restorations last decades.
Maintenance includes:
- Professional cleanings
- Night guards
- Regular examinations
Long-term studies show implant-supported restorations can last over 20 years.
Final Section: Why Full Mouth Rehabilitation Restores Health, Function, and Facial Structure
Full mouth rehabilitation restores structural stability, jaw alignment, and oral function while improving facial proportions and quality of life.
Modern implant dentistry, digital planning, and prosthetic materials allow predictable, durable outcomes.
Patients seeking permanent restoration of oral function and facial support benefit significantly from full mouth rehabilitation performed by experienced restorative specialists.