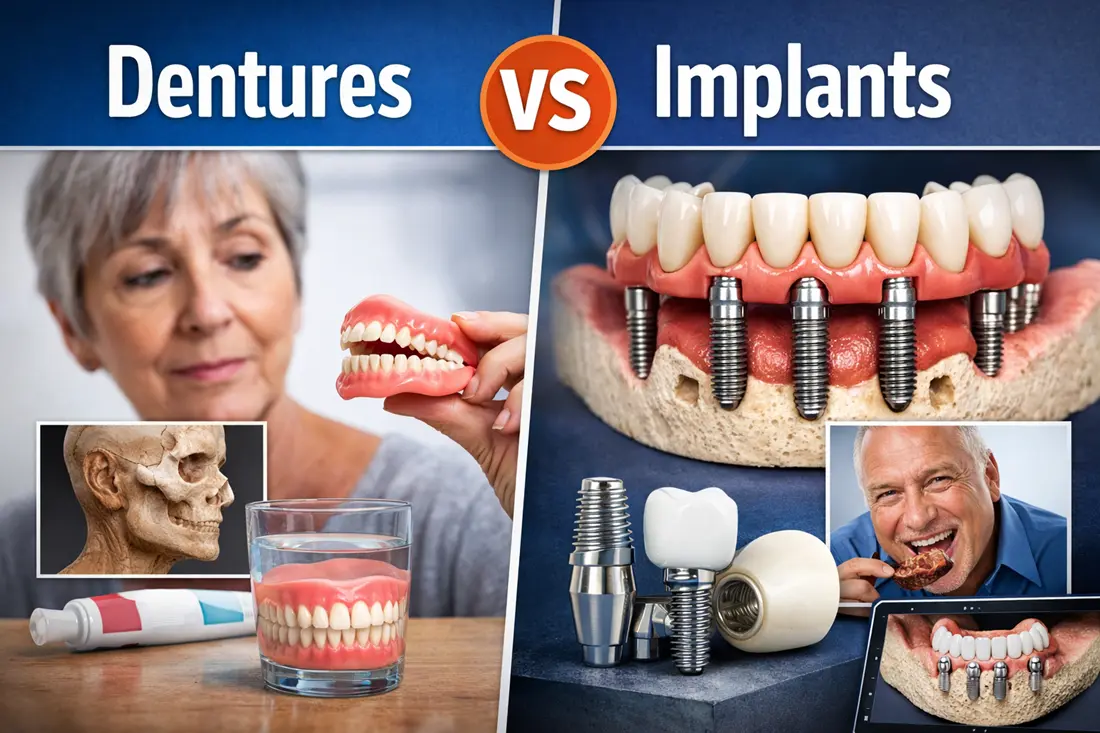
Dentures vs. implants is the decision that looks simple on a brochure and gets very real the first time you try to bite into something that fights back.
If you’re here because you want the honest version (not the “everything is amazing” version), you’re in the right place. We’ll cover the costs you don’t see on day one, the biology nobody explains well, and the practical stuff that actually affects your life: chewing, speech, comfort, confidence, repairs, and long-term upkeep.
Why is there such a massive price difference between dentures and implants?
Dentures vs. implants pricing feels unfair because you’re not buying the same thing.
Dentures are a removable prosthesis that rests on gum tissue (and sometimes remaining teeth). The materials and lab work matter, but the core design still relies on soft tissue support and suction.
Implants are titanium (or titanium-zirconium) fixtures placed in bone to support crowns, bridges, or overdentures. You’re paying for surgical planning, sterile protocols, hardware, restorative parts, lab manufacturing, follow-ups, and risk management.
A good rule: dentures are more “device + adjustments.” Implants are more “procedure + engineering + maintenance.”
Does wearing dentures lead to permanent facial structure changes?
Yes, it can. Not because dentures are “bad,” but because missing tooth roots change bone behavior.
When teeth (roots) are gone, the jaw no longer gets normal stimulation from biting forces through the periodontal ligament. Bone remodeling trends toward resorption over time, especially in the lower jaw.
Long-term classic prosthodontic research tracked continued residual ridge reduction in complete denture wearers over extended periods.
A well-known longitudinal study on complete denture changes also exists in Acta Odontologica Scandinavica.
What that can look like in real life
- The lower denture gets looser as the ridge flattens
- Lips lose support, corners of the mouth fold inward
- Chin appears closer to the nose (“collapsed” lower face height)
- The “sunken face” look becomes more likely if fit and bite are not maintained
What happens to your jawbone when there are no tooth roots?
Your jawbone is not sentimental. If it’s not being used like it used to be, it tends to shrink.
Here’s the practical point: dentures sit on the ridge, and the ridge may reduce over time. Implants load the bone, which can help maintain function and support around the implant sites (not a guarantee, but a different biological situation).
Implant success evaluations often track marginal bone level changes, commonly discussed as early remodeling with tighter thresholds later on.
Which option looks more natural under bright, direct sunlight?
Under harsh lighting, the tell is usually not “implant vs denture.” It’s:
- tooth shape and translucency
- gum contour realism
- lip support
- how stable the teeth look when you talk and laugh
Dentures can look extremely natural when designed well. The risk is that movement and loss of lip support over time can give away the “denture look.”
Implant bridges can look highly natural too, though some fixed full-arch designs trade a little “gum realism” for hygiene access and structural strength.
Is “Denture Breath” a real thing, and can it be prevented?
It can be real, and it’s usually not mysterious.
Common causes:
- biofilm on the denture surface (especially the tissue side)
- sleeping with dentures in
- dry mouth
- inadequate cleaning of the tongue and gums
A professional cleaning schedule matters because plaque isn’t loyal to natural teeth only. If you need a baseline plan for preventive care, this is where routine hygiene and exams support everything else: Dental Cleanings.
Why do dentures need “Relines” every few years?
Because your mouth changes, and acrylic doesn’t magically change with it.
A reline refits the denture base to match the current ridge shape. Without it, you get:
- rocking and sore spots
- reduced suction
- more adhesive dependency
- higher risk of cracks from uneven load
Relines are normal maintenance, not a “failure,” but they are part of the lifetime cost.
Dentures vs. Implants cost in 2026, what people forget to calculate
Dentures vs. implants cost is not a single number. It’s a timeline of expenses: initial treatment, follow-ups, repairs, relines, replacement cycles, hygiene visits, and complication management.
Figure 1: Typical lifetime-cost categories (illustrative ranges)
Real fees vary by region, materials, surgical needs, and insurance. This table is meant to show where costs come from, not to quote your exact total.
| Cost category | Conventional full dentures | Implant overdenture (“snap-in”) | Fixed full-arch implant bridge |
|---|---|---|---|
| Initial prosthesis and delivery | Lower | Medium | Highest |
| Adjustment visits (first 90 days) | Common | Common | Common |
| Relines over time | Common | Sometimes | Rare |
| Adhesives and daily products | Common | Usually reduced | Usually none |
| Repairs (cracks, tooth wear) | Sometimes | Sometimes | Sometimes |
| Surgical procedures | None | Yes | Yes |
| Long-term complication management | Tissue soreness, looseness | Attachment wear, hygiene | Hygiene access, mechanical parts |
If you want to explore the denture options spectrum (traditional, partials, premium materials), start here: Dentures.
If your real concern is “I want stability but I’m not ready for fixed,” this is the middle lane: Implant-Supported Dentures.
The “Plastic Taste” factor: How dentures change your relationship with food
Upper dentures often cover part of the palate, which can influence texture perception and sometimes taste experience. Research on palatal coverage shows measurable effects on oral perception.
Clinical research has also evaluated gustatory and olfactory changes in complete denture wearers.
Practical ways patients reduce this issue:
- thinner palatal design when clinically appropriate
- stable fit (less movement = less “foreign body” feeling)
- keeping the denture surface clean (biofilm can alter taste and smell)
- considering implant retention when stability is the main problem
Why do some people experience “Denture Slur” when speaking?
Speech is muscle memory plus tongue space. Dentures can change both.
Common triggers:
- slightly thick acrylic in the wrong places
- unstable denture movement on “s,” “t,” “d,” and “sh” sounds
- altered bite height
- too much palatal coverage for that individual
This is why the “adjustment period” is real, and why a clinician who does careful phonetic checks is worth more than a coupon.
What your dentist might not tell you about the “adjustment period”
Here’s what usually happens (and what should not happen).
Normal early experiences
- mild sore spots
- extra saliva
- “full mouth” feeling
- some chewing awkwardness
Not normal
- ulcers that don’t improve with adjustments
- persistent rocking after multiple visits
- major bite imbalance that causes jaw pain
- repeated cracks from the first weeks
If you’re repeatedly returning for pain relief, that’s not “your mouth being difficult.” That’s a fit/occlusion problem that needs better correction.
Dentures vs. Implants and the hidden biology nobody explains well
Dentures vs. implants is really a question about where forces go.
- Dentures send force into soft tissue and residual ridge
- Implants send force into bone at implant sites
- Natural teeth distribute force through periodontal ligament (a shock absorber dentures don’t have)
That leads to one of the most important technical realities:
Five technical details that actually matter
- Osseointegration: implant stability depends on bone healing directly to the implant surface.
- Insertion torque and primary stability influence immediate vs delayed loading decisions (your dentist is measuring this).
- Marginal bone level changes are tracked around implants over time as part of health monitoring.
- Attachment systems (locator-type, bars, magnets) wear over time in overdentures and require maintenance.
- Peri-implant diseases exist: mucositis and peri-implantitis are real risks and need ongoing hygiene. Large systematic reviews report meaningful prevalence figures over time.
So yes, implants can feel stable, but they are not “set it and forget it.” The maintenance myth hurts patients.

Dentures vs. Implants: Which option protects your jawbone and facial support better?
Dentures vs. implants affects jawbone support because the forces you apply when chewing either load the bone (implants) or sit mainly on soft tissue (dentures), and that difference can show up in facial support over time.
When tooth roots are missing, the jawbone often remodels and may reduce over the years, which can change denture stability, lip support, and lower-face height. Implant-supported options can help create more stable function at the implant sites, but they still require careful planning, hygiene, and follow-up.
What this means in real life
- If you’re worried about a “sunken” look, you should think about support and stability, not just tooth color and shape.
- If you already wear dentures, periodic relines and bite checks matter because changes can be gradual and easy to ignore until the denture feels “off.”
- If implants are planned, bone volume and gum health still decide how predictable the outcome is.
Quick question to ask in consultation:
“Which parts of my facial support come from denture design versus bone level, and how do we plan to keep that stable?”
Can you really eat steak with dentures? The honest truth.
Some people can. Many people start with steak as the fantasy and end up choosing:
- softer cuts
- smaller bites
- slower chewing
- avoiding tough foods in public
Chewing efficiency often improves with implant support. A 2019 systematic review found strong 10-year implant survival estimates, which helps explain why implant-supported solutions are commonly chosen when chewing function is the top goal.
Patient-centered outcomes often show higher satisfaction and function scores for implant overdentures compared with conventional dentures.
No, this doesn’t mean dentures “don’t work.” It means physics has opinions.
H2: Dentures move; implants stay. But is the price gap worth it?
Dentures can move because they rely on suction, ridge shape, saliva, and muscle control, while implant options gain retention from hardware anchored to bone. The price gap feels big because you’re paying for very different systems.
What’s the real “movement tax” you pay with dentures?
Movement often shows up as:
- slower eating and smaller bites
- more time spent on adhesives or refitting
- sore spots from friction
- social anxiety about speaking or laughing freely
When does the gap feel “worth it” to patients?
Common tipping points are:
- frustration with daily adhesives
- lower denture instability
- frequent relines/adjustments
- difficulty chewing protein foods
10 years later: Which investment actually holds its value?
Ten years later, many patients judge value by how stable their daily life feels: chewing comfort, social confidence, and how often they need repairs, relines, or remakes.
The “lifetime cost” buckets people forget
- Denture relines and remakes
- Repairs from cracks or worn teeth
- Adhesives and daily maintenance products
- Follow-up visits for fit, bite, sore spots
- Implant maintenance visits and part replacement (attachments, screws, wear items)
The psychological toll of “floating” teeth vs. fixed roots
Confidence is not vanity. It’s the ability to eat, laugh, and speak without constantly checking your teeth. Many people who feel their dentures “float” describe a background stress that shows up in public meals and conversations.
Small daily moments where stability matters most
- ordering food without fear
- speaking clearly during meetings
- smiling in photos without “holding back”
- not avoiding crunchy or chewy foods in public
Why “Snap-in” dentures are the middle ground nobody talks about
Snap-in dentures (implant overdentures) often give a noticeable stability boost without the complexity and cost of a full fixed bridge. They can be a practical compromise when you want less movement but also want removability for cleaning.
Why clinics often see higher acceptance for this option
It usually feels like a “reasonable step up”: more stable than suction dentures, typically less expensive than full fixed arches, and many patients understand the value quickly after they experience retention.
The real reason some dentists push implants over traditional plates
This topic needs a fair tone. It’s not “dentists hiding secrets,” it’s a mix of clinical goals, patient outcomes, and how dentistry is practiced.
Common reasons implants get recommended more:
- more stable chewing and speech outcomes for many patients
- predictable retention options for difficult lower dentures
- patient demand for fixed-feeling teeth
- long-term maintenance planning that can reduce repeated denture remakes
Also true: implants are not ideal for everyone, and good clinicians should present a real options ladder, not a single “one-size” plan.
Speech hurdles: Relearning to talk with a palate-covered mouth
Speech changes happen because dentures change tongue space, airflow, and the palate’s surface. Most people adapt, but the first days and weeks can feel awkward.
Simple practice plan that helps many patients
- read aloud 5 minutes daily
- repeat “sixty-six,” “Mississippi,” and “thirty-three” slowly
- schedule early adjustments if specific sounds trigger clicking or slipping
Your 2026 guide to making the final decision for your smile
Decision clarity comes from matching your anatomy, medical risks, timeline, and maintenance comfort level to the right option, not from chasing the “most expensive” solution.
Healing Timelines: What happens in Week 1 vs. Month 6?
In many cases, dentures vs. implants comes down to timing: dentures can be delivered fast, while implants usually need healing time for stable bone integration.
Week 1: What most patients feel and notice
- Immediate denture (same-day): you can leave with teeth the same day in selected situations, but swelling changes the fit quickly, so early adjustments are common.
- Implant placement: soreness and swelling can happen, and your dentist may recommend soft foods and careful cleaning.
Month 2 to Month 6: Why implants take longer
A key step for implants is osseointegration, which often takes about 3 to 6 months in many treatment plans. During this time, bone bonds to the implant surface, creating stability that supports chewing forces.
The trade-off that’s easy to miss
- Immediate dentures give speed, but they often need more adjustments as healing reshapes the ridge.
- Implants take longer, but the goal is more predictable stability once healed.
The Middle Ground: How 2–4 implants can turn a loose denture into a stable solution
Many people assume the choices are either a traditional denture or a full fixed implant bridge. The middle options are often the most practical.
What changes when you add just 2 implants
For many lower dentures, adding 2 implants can dramatically improve retention using overdenture attachments. It does not turn it into a fixed bridge, but it can reduce slipping and adhesive dependence.
What changes when you use 4 implants
With 4 implants, some patients can qualify for designs that feel more stable and distribute forces better, depending on anatomy and prosthesis type.
Why this “middle option” often converts well
Patients often like it because:
- it feels like a real stability upgrade
- it is usually more affordable than full fixed arches
- it still allows removability for easier cleaning
Self-Assessment: Am I a better fit for implants or dentures?
This quick checklist helps you clarify which option matches your comfort level, timeline, and health factors. It does not replace an exam, but it helps you ask better questions.
Checklist for Implants
| Statement | Yes / No |
|---|---|
| I don’t smoke (or I’m willing to quit/reduce significantly). | |
| I can commit to daily cleaning and regular maintenance visits. | |
| I’m comfortable with a surgical procedure if I’m cleared medically. | |
| I can plan for a longer treatment timeline (often months). | |
| I’m choosing a long-term stability goal, not just speed. | |
| I understand implants still need ongoing care (not “done forever”). |
Checklist for Dentures
| Statement | Yes / No |
|---|---|
| I want a non-surgical approach. | |
| I need teeth delivered quickly (speed matters most). | |
| I’m okay with adjustments and relines over time. | |
| I’m comfortable removing the denture for cleaning. | |
| My budget is tighter upfront. | |
| I’m okay with learning techniques to manage movement. |
Tip for better consults: bring this checklist and ask your dentist which “No” answers are deal-breakers and which can be improved with treatment planning.
Why do some implants fail while others last a lifetime?
Implant outcomes depend on site biology, habits, and execution.
A widely cited systematic review estimated 10-year implant-level survival around 96.4% (with prediction intervals showing variability).
Long-horizon reviews have also summarized 20-year survival outcomes, noting that long follow-up is complicated and failures still happen.
Common risk factors in real clinics:
- smoking
- uncontrolled diabetes
- poor plaque control
- history of periodontitis
- bruxism (clenching/grinding)
- thin bone or poor bone density
- inadequate maintenance visits
Can systemic health issues like diabetes disqualify you from implants?
Sometimes. Not always.
Well-managed diabetes may still allow implant treatment, but risk management becomes stricter. This is a medical discussion, not a marketing claim, and it’s one reason a thorough exam matters.
What are the “Hidden Risks” of oral surgery for seniors?
Age alone is not the whole story. The real variables:
- anticoagulants and bleeding risk management
- immune status and healing capacity
- bone quality
- dexterity for hygiene (implants still need cleaning)
- ability to attend follow-up visits
A safe plan is individualized, with medical coordination when needed.
Is the recovery period for implants as painful as people say?
Most patients describe it as manageable with proper planning and meds, but the honest answer is: recovery varies.
What drives a rougher recovery:
- bone grafting volume
- sinus lift procedures
- multiple implants placed at once
- untreated inflammation or infection at baseline
Immediate-load full-arch studies report high early survival in many protocols, but they still track failures and bone changes.
How long does the “Implant trip” actually take from start to finish?
Typical phases:
- Exam, imaging, and treatment planning
- Extractions or site prep if needed
- Implant placement
- Healing / integration period
- Final prosthesis fabrication and delivery
- Maintenance schedule
The timeline ranges from weeks (selected immediate protocols) to months (grafting, staged approaches). Anyone promising “everyone finishes fast” is selling, not planning.
Are “All-on-4” implants really better than traditional dentures?
“All-on-4” can be excellent for the right patient, but “better” depends on goals and risk tolerance.
Clinical research continues to track full-arch outcomes with strong reported survival in many cohorts.
Also keep your eyes open for complications beyond survival numbers, because repairs and biologic issues affect lived experience.
If you’re comparing fixed full-arch options, see: Fixed Hybrid Dentures.
How do “Snap-In” dentures compare to traditional “Suction” dentures?
Snap-in dentures (implant overdentures) usually give:
- noticeably more retention
- less rocking during chewing
- reduced adhesive use
- better confidence during speech and social eating
Patient-reported outcomes frequently show higher satisfaction and comfort with implant overdentures compared to conventional dentures.
The trade-offs:
- attachment parts wear and need replacement
- hygiene needs more discipline
- implants still require monitoring for inflammation
Can you switch from dentures to implants after 10 years of bone loss?
Sometimes yes, sometimes no, sometimes “yes but with grafting.”
Residual ridge reduction over time is documented in long-term prosthodontic literature.
The longer someone is edentulous, the more likely advanced site development is needed.
If you’re trying to plan a “phase approach,” ask about:
- implant overdenture as a first step
- staged grafting
- fixed full-arch only if hygiene access and risk profile fit
Surgery anxiety vs. daily adhesive: Which “pain” can you live with?
This is a real quality-of-life question, not a dental trivia question.
Some people would rather do:
- one planned surgical phase
than deal with: - daily adhesives
- fear of movement
- repeated sore spots
- public eating anxiety
Others prefer:
- no surgery
- removable simplicity
- faster upfront completion
Neither choice is morally superior. It’s just your tolerance profile.
Emergency repairs: What happens when a denture snaps at dinner?
It happens. Usually at the worst time, because humans are not allowed peace.
Common causes:
- thin acrylic zones
- bite imbalance creating stress points
- dropping the denture in a sink
- older denture teeth wearing down and changing force patterns
Plan ahead:
- ask if your clinic offers repair support
- have a travel case
- avoid “DIY glues” that are not intended for intraoral use
How do you handle a “Denture Emergency” while traveling?
Simple checklist:
- bring the case and a soft brush
- pack adhesive if you use it
- carry a small container for soaking (hotel cups are… not ideal)
- avoid wrapping in napkins (most dentures are lost this way)
If your denture is implant-retained, bring any tools your clinician recommends for inserts or cleaning.
How modern 3D printing is closing the gap between dentures and implants
Digital dentures are not magic, but they can improve consistency, remake speed, and sometimes fit predictability.
A 2024 clinical outcomes review discussed 3D-printed complete dentures and patient-based outcomes.
A 2025 systematic review assessed patient satisfaction for CAD/CAM 3D-printed complete dentures versus conventional.
Digital does not remove the need for:
- good impressions or accurate scans
- correct bite records
- skilled tooth setup and occlusion
It just changes the manufacturing pathway.
Why some patients actually prefer high-end partials over surgery
If someone has stable remaining teeth, a well-designed removable partial denture can be:
- less invasive
- easier to repair
- financially manageable
- fast to complete
The key is selection and design. Bad partial designs can damage supporting teeth. Good ones protect them.
Is your jawbone strong enough for implants? The deal-breaker.
This is where imaging matters (often CBCT), and where honesty matters even more.
Your clinician is evaluating:
- bone height and width
- density and cortical thickness
- proximity to nerves and sinuses
- bite forces and parafunction
- gum and bone health history
If implants are not ideal today, that does not mean “never.” It means you plan the steps that make them safer.
Which choice provides the best long-term ROI for your confidence?
This question is emotional, but it has practical inputs:
Confidence tends to track with:
- stability (movement anxiety is a thief)
- speech reliability
- ability to eat comfortably in public
- appearance consistency over time
- low drama maintenance
Implant overdentures and fixed implant bridges often score higher in satisfaction measures in many studies.
That said, a well-made denture that fits properly and is maintained well can still be life-improving.
Where does full-mouth rehab fit when the situation is complex?
If you have a mix of missing teeth, worn teeth, bite collapse, and failing restorations, the decision might not be “denture vs implant” alone.
That’s when broader planning can matter: Full Mouth Rehabilitation.
WHO should consider each option, and WHICH questions decide it fastest?
Dentures tend to fit best when:
- you want no surgery
- you need a faster start
- medical risk makes surgery high-risk
- you’re comfortable with removables and maintenance visits
Implants tend to fit best when:
- stability is the top priority
- you want improved chewing and speech confidence
- you can commit to hygiene and follow-ups
- bone volume and health profile are favorable
Snap-in overdentures fit best when:
- lower denture stability is a major problem
- you want a middle-cost approach
- you want removability for easier cleaning
You can review denture paths here: Dentures and stability-focused options here: Implant-Supported Dentures.
Still Unsure? Let’s Break It Down Together
Dentures vs. implants isn’t a one-size-fits-all decision. A quick exam and digital scan can reveal whether stability, bone support, or cost should guide your choice.
📞 Call now (562) 242‑1411 or book online to get a customized treatment plan designed around your comfort and long-term results.